Types of Skin Cancer
Skin cancer is a general term for all malignant changes in the skin. Depending on which type of skin cell is damaged and how malignant is the cancer, it can be divided into different types, each one having different characteristics.
Skin cancer is a general term for all malignant changes in the skin. It develops primarily on areas exposed to the sun such as the scalp, face, lips, ears, neck, chest, arms, and hands. Skin cancer affects people of all skin tones, including those with darker complexions.
Depending on which skin cell is damaged first and how malignant is the cancer is, it can be divided into different types, each one having different characteristics.
The two main types of skin cancer are Melanoma and Non-Melanoma skin cancer, they both originate in the epidermis. The epidermis is the outermost layer of skin on the body.
Both Melanoma and Non-Melanoma skin cancers originate in the epidermis.
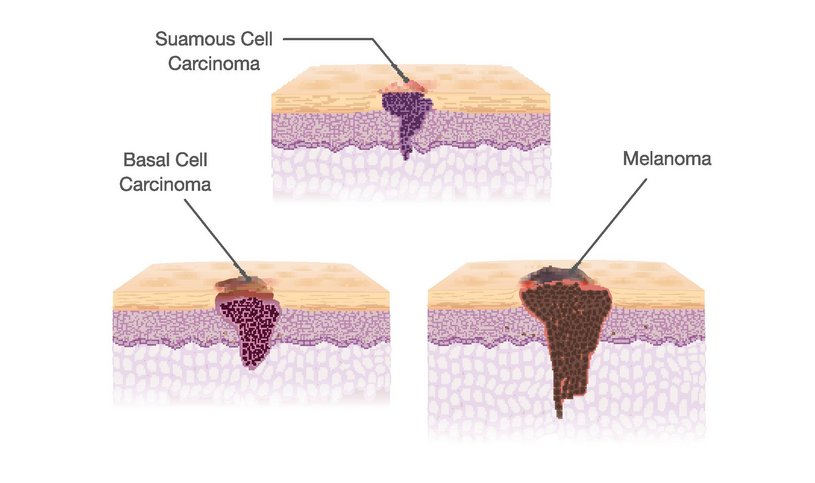
Non-melanoma skin cancers can be further categorized as either Basal or Squamous cell carcinomas;
Basal cell carcinomas (BCCs) ariseevolve from basal cells in the epidermis when start an abnormal uncontrolled growth. Most BCCs are caused by cumulative, long-term exposure to UV radiation from the sun and can be very destructive if they are not detected early enough.
Squamous cell carcinomas (SCC) arise from squamous cells in the epidermis when they start growing in aan uncontrolled manner due to long-term UV radiation exposure. SCCs can sometimes grow quickly and could metastasize if they are not treated early.
Melanoma originates in the melanocytes, the cells that produce melanin and give colour to the skin, which they are located in the bottom layer of the epidermis. Melanoma is more dangerous than non-melanoma skin cancer, as it can metastasize quickly and spread to other organis if not detected and treated at an early stage.

