Risk Factors
UV-radiation is the main cause for Skin Cancer, but it is not the only risk factor. Your skin type also plays a decisive role in the sensitivity to UV rays as well as your genes do.
UV-Radiation
It is estimated that 90% of all non-melanoma skin cancers (NMSC) are due to frequent and intensive sun or solarium exposure of the skin1. Thus, sun or solarium irradiation are the main risk factors of light skin cancer.
The component from sunlight that causes skin cancer is ultraviolet radiation (UV-radiation), an electromagnetic radiation which is invisible to the human eye. There are types of UV-radiation: UVA, UVB and UVC radiation.
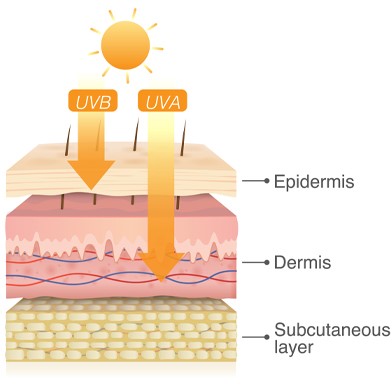
While UVA and UVB rays are transmitted through the atmosphere, all UVC and some UVB rays are absorbed by the Earth’s ozone layer. So, most of the UV rays you come in contact with are UVA with a small amount of UVB, which are characterized for having different penetration depths into human tissue due to their different physical properties:
- UVB rays have a short wavelength that reaches the outer layer of your skin (the epidermis)
- UVA rays are lower in energy than UVB but have a longer wavelength that can penetrate the middle layer of your skin (the dermis).
Therefore, UVA rays can penetrate right into the dermis and are largely responsible for skin aging. UVB rays have a lower penetration depth and they only reach the epidermis, however, they are more energetic and the impact they have on the skin cells is higher. They are, therefore, mainly responsible for the development of Skin Cancer.
Type of Skin
Each skin type plays a decisive role in the sensitivity of the skin to UV rays. Depending on UV sensitivity, 6 skin types are distinguished, which can be traced back to the 1975 classification by the American dermatologist Thomas Fitzpatrick2,3
| Type | Name | Physical Characteristics | Description |
| I | Light | Eyes: Blue Hair: Blond Skin: Porcelain | Very sensitive to UV-radiation. Never gets tan and gets sunburnt very quickly. |
| II | Fair | Eyes: Grey, green, brown Hair: blonde to brown Skin: light, sensitive | Hardly tans at all to moderately and often gets a sunburn. |
| III | Medium | Eyes: grey or brown Hair: dark blonde to brown Skin: light to tan | Sometimes mild burn, tans uniformly |
| IV | Mid Brown | Eyes: brown to dark brown Hair: dark brown Skin: light brown olive skin | Rarely burns and tans quickly. |
| V | Dark Brown | Eyes: Dark brown Hair: Dark brown to black Skin: dark brown skin | Moderately pigmented brown skin, very rarely burns and tans very easily. |
| VI | Very Dark Brown | Eyes: Dark brown Hair: Black Skin: dark brown to black | Deeply pigmented dark brown to black skin; never burns, tans very easily |
Medication
Besides UV-radiation, some drugs might also play a role in the development of skin cancer.
Many drugs including tetracyclines, fluoroquinolones, nonsteroidal anti-inflammatory agents (like aspirin or ibuprofen) are known to have photosensitizing properties. There is evidence that photosensitisation of the skin that is being exposed to UV-radiation can enhance the risk of sunburns and damage the skin, which might increase the risk of skin cancer 4.
In addition, Immunosuppressive drugs for example, which are often given after an organ transplant to suppress a rejection reaction, can also affect our own’s body defence to fight against cancer 5.
Hereditary disease
Hereditary diseases can also promote the development of skin cancer. The basal cell carcinoma syndrome, also known as Gorlin-Goltz syndrome or basal cell nevus syndrome, can be the trigger for the development of basal cell carcinomas.
Albinism, xeroderma pigmentosum (moonlight disease), Muir-Torre syndrome or epidermolysis bullosa (butterfly skin) are inherited syndromes that can increase the risk for the development of NMSC 6.
References
1. InYoung Kima and Yu-Ying Heb. Ultraviolet radiation-induced non-melanoma skin cancer: Regulation of DNA damage, repair and inflammation. Genes & diseases. 2014; 1: 188-198.
2. Besundesamt für Strahlenschuty. Optische Strahlung: UV-Strahlung – Sonne – Solarien – Infrarot-Strahlung – Laser. [Available at: http://www.bfs.de/DE/themen/opt/uv/wirkung/hauttypen/hauttypen.html].
3. Widemar K and Falk M. Sun Exposure and Protection Index (SEPI) and Self-Estimated Sun Sensitivity. The Journal of Primary Prevention. 2018; 39: 437-451.
4. Kaae J, et al. Photosensitizing Medication Use and Risk of Skin Cancer. Cancer Epidemiol Biomarkers Prev. 2010; 19(11): 2942-2949.
5. Kuijken I, Bavinck JN. Skin cancer risk associated with immunosuppressive therapy in organ transplant recipients: epidemiology and proposed mechanisms. BioDrugs. 2000;14(5):319-329.
6. Jaju PD, et al. Familial skin cancer syndromes: Increased risk of non-melanocytic skin cancers and extracutaneous tumors. J Am Acad Dermatol. 2016; 74(3): 437-454.