Non-Melanoma Skin Cancer - what are the treatment options?
Dear readers,
Welcome to the NMSC Blog!
As you probably already know, non-melanoma skin cancer or NMSC is the most common cancer in the world.
The good thing is, if it is early diagnosed, it can be easily treated.
Today we will talk about some of the therapies available for skin cancer which may help you decide, together with your doctor, which is the best therapy option for you.
Microscopically Controlled Surgery
Sometimes also called Mohs surgery, is done in different stages: The surgeon cuts the first layer of cancerous tissue, including a small margin of surrounding healthy tissue (also called safety margin). Right after, the laboratory analyses it, while the patient waits. If any cancer cells remain at any of the edges, additional skin tissue is removed in stages and examined under the microscope until no more cancer cells are present. Once the area is clear, the wound is closed which, in some cases, may need reconstruction. Depending on the size and depth of the original lesion, skin grafting may be necessary to ensure the proper aesthetic result.
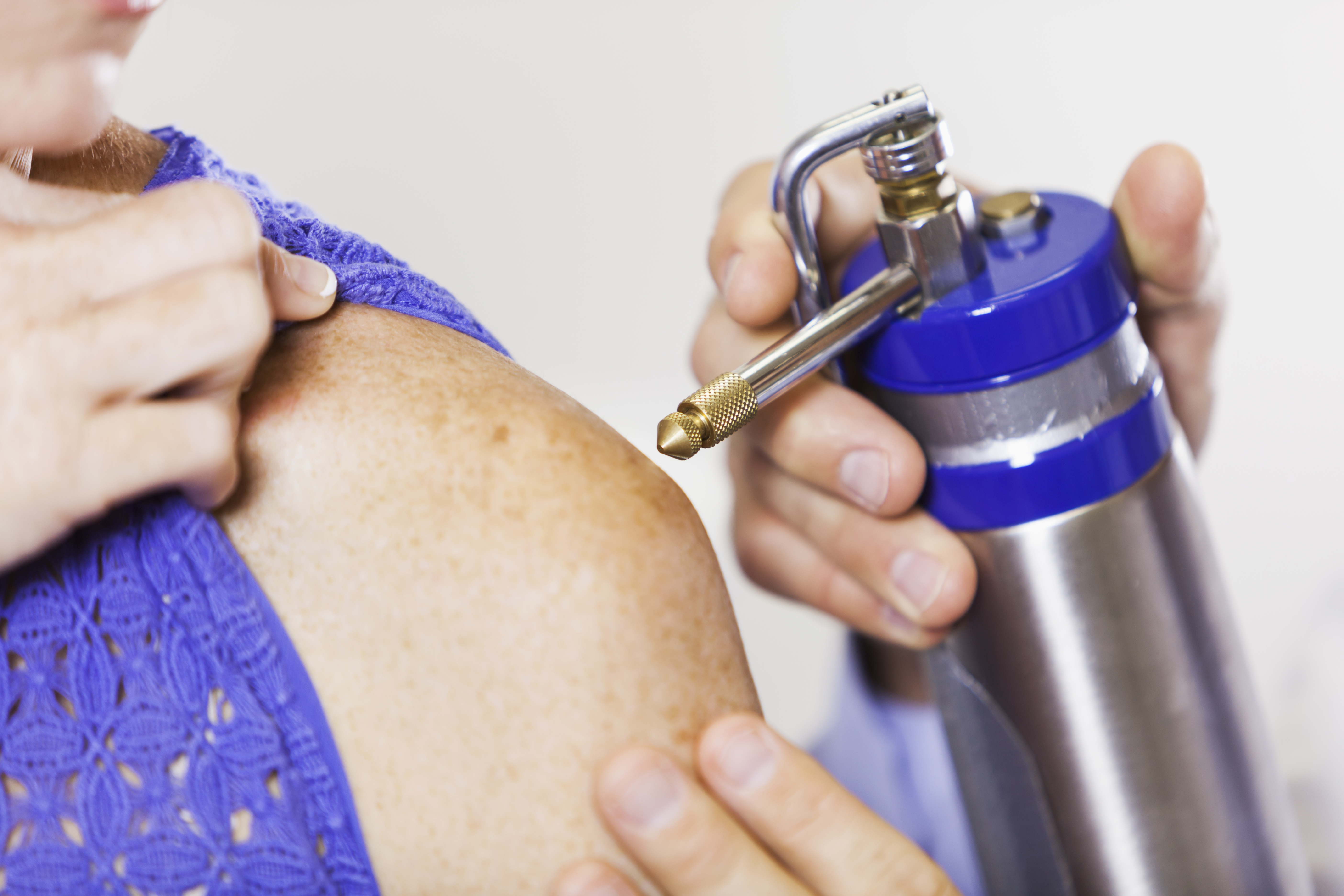
Curettage and electrodessication
This is a procedure commonly performed by dermatologists and surgeons for the treatment of very superficial basal cell and squamous cell carcinomas. During the procedure, the doctor will scrape the affected area with a curette (a spoon-shaped instrument) and optionally, once the cancerous tissue has been removed, the doctor will cauterize the area (also called electrodessication).
Unfortunately, as the excised tissue has been scraped off, it is difficult to examine it under the microscope. This is why the recurrence of this treatment tends to be higher1.
Photodynamic therapy (PDT)
PDT is used to treat large, superficial tumours. It uses a cream (called photosensitizer drug) that is applied over the tumour to make cancer cells and other abnormal cells vulnerable to a high energy light. When the tumour area is exposed to this type of light, the photosensitizer drug gets activated, it becomes toxic to cancer cells and they die. During the procedure, some patients tend to feel some pain.
Radiation Therapy
Radiation therapy uses primarily x-rays to destroy cancer cells. It is painless and may be used when surgery is a less suitable option - if a tumour is very large or is on an area of the skin that makes it hard to remove with surgery.
There are different types of radiation therapy:
- External Beam radiation: When the radiation is given from a machine that directs the radiation to a part of the body where the cancer is located.
- Brachytherapy: When the radioactive material is placed very closed to the cancer lesion (from the inside or the outside).

What is the effect of radiation?
Radiation damages the DNA of cancer cells. They can’t grow and divide anymore, which end up dying.
Classic radiation therapies like external beam radiation that use X-Rays, tend to irradiate bigger areas, which could affect not only the tumour but also the healthy tissue surrounding it. Thus, to administer the necessary dose of radiation whilst minimising side effects and damage to normal tissue, the radiotherapy must be delivered over a number of sessions. For this reason, radiation therapies are usually performed in multiple sessions over several weeks (4-7 weeks).

How does brachytherapy work differently?
Brachytherapy treatment delivers radiotherapy close to the skin area of the tumour and to a small area of normal tissue around the tumour.
One example of brachytherapy is the Rhenium-SCT, which uses the isotope Rhenium-188 that emits beta-radiation and damages the DNA of the cells. These isotopes are placed directly next to the tumour tissue and then removed. Since the radioactive material is placed very closed to the cancer lesion, the treatment destroys the tumour cells without compromising the surrounding healthy tissue.
Some radioactive isotopes such as Rhenium-188 have an effect only in the first 2-3 mm of skin. These type of radioisotopes are ideal to treat superficial tumours such as skin tumours. In the case of the Rhenium-SCT, the radioactive source is located inside a liquid paste and placed directly over the tumour, which makes it ideal to treat parts of the body that are difficult to reach (like the nose or the ears).
Hopefully this short overview of the most common treatment options has clarified some of your questions. If you need medical advice or more detailed information, reach out to your doctor.
If you found this post useful and would like to know more, subscribe to the blog or follow us on social media!
Literature
- Chren M-M, et al. Tumor Recurrence 5 Years after Treatment ofCutaneous Basal Cell Carcinoma and SquamousCell Carcinoma. Journal of Investigative Dermatology. 2013; 133: 1188-1196.

